Proton Services | Access Specialists
Apollo Healthcare has refined a process that has achieved a 70% success rate for specialties that typically receive a 10% success rate. We use clinically trained and board certified experts to navigate every authorization. On average our team submits over 30 pages of clinical justification to your patient’s insurance company. Every case is tailored to your patient’s specific needs. No templates, every authorization is pursed in a unique fashion.
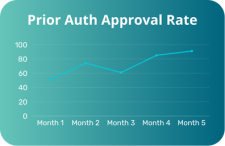


Our expertise in radiation oncology has led to significant improvements for our clients. By efficiently managing prior authorizations, we’ve helped practices reduce delays and enhance patient satisfaction.
Don’t let administrative hurdles delay critical cancer treatments. Contact us today to discover how our prior authorization services can expedite patient care in radiation oncology.