Prior Authorization
In the field of radiation oncology, timely treatment is crucial for patient outcomes. Prior authorizations can often delay the start of essential therapies, impacting patient care. At Radiation Business Solutions (RBS), we specialize in simplifying the prior authorization process specific to radiation treatments. Our dedicated team navigates the complexities on your behalf, ensuring swift approvals so you can focus on delivering life-saving care to your patients.
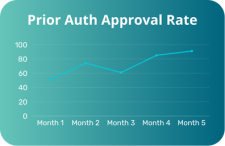


Our expertise in radiation oncology has led to significant improvements for our clients. By efficiently managing prior authorizations, we’ve helped practices reduce delays and enhance patient satisfaction.
Don’t let administrative hurdles delay critical cancer treatments. Contact us today to discover how our prior authorization services can expedite patient care in radiation oncology.